Contents
- 1 Epidural vs Spinal: Understanding the Differences and Benefits
- 1.1 What is Epidural Anesthesia?
- 1.2 What is Spinal Anesthesia?
- 1.3 Differences between Epidural and Spinal Anesthesia
- 1.4 FAQ about topic Epidural vs Spinal: Understanding the Differences and Benefits
- 1.4.1 What is the difference between an epidural and a spinal?
- 1.4.2 Which type of anesthesia is more effective for pain relief during childbirth?
- 1.4.3 Are there any risks or side effects associated with epidurals and spinals?
- 1.4.4 Can I choose between an epidural and a spinal for my childbirth?
- 1.4.5 How long does the pain relief last with an epidural compared to a spinal?
- 1.4.6 What is the difference between an epidural and a spinal block?
- 1.4.7 Are epidurals and spinal blocks used for the same purposes?
- 1.4.8 What are the benefits of an epidural?
- 1.4.9 What are the potential risks and side effects of a spinal block?
- 1.4.10 Can anyone receive an epidural or spinal block?
Epidural vs Spinal: Understanding the Differences and Benefits

When it comes to managing pain during labor or certain medical procedures, two common options are epidural and spinal anesthesia. Both methods involve the injection of medication into the spine, but there are important differences between the two.
An epidural is a type of regional anesthesia that is commonly used during childbirth. It involves the placement of a catheter in the epidural space, which is the area surrounding the spinal cord. The medication is then delivered through the catheter, providing pain relief by numbing the nerves in the lower half of the body. This allows the mother to remain awake and alert during labor while experiencing reduced pain.
On the other hand, spinal anesthesia is a single injection of medication directly into the cerebrospinal fluid in the spinal canal. This type of anesthesia is commonly used for surgeries below the waist, such as cesarean sections or hip replacements. It provides a more intense and immediate blockage of pain sensation, but it also has a shorter duration of action compared to an epidural.
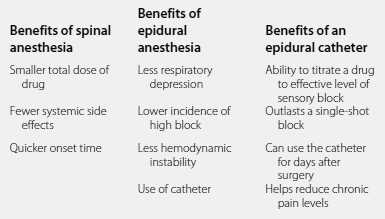
Both epidural and spinal anesthesia have their own set of benefits and potential complications. An epidural can provide long-lasting pain relief, allowing the mother to rest and conserve energy during labor. However, it can also cause side effects such as low blood pressure or difficulty urinating. Spinal anesthesia, on the other hand, offers a quicker onset of pain relief and a lower risk of complications. However, it can also cause temporary numbness or weakness in the legs.
Ultimately, the choice between epidural and spinal anesthesia depends on the specific needs and preferences of the patient, as well as the recommendations of the anesthesiologist. It is important to discuss the options and potential risks with your healthcare provider to make an informed decision about pain management during labor or surgery.
What is Epidural Anesthesia?
Epidural anesthesia is a medical procedure commonly used during childbirth or surgery to provide pain relief. It involves the administration of anesthesia by an anesthesiologist through an injection into the epidural space, which is the area surrounding the spinal cord.
During the procedure, the anesthesiologist will insert a small needle into the lower back, carefully guiding it into the epidural space. A catheter may then be threaded through the needle, allowing for continuous administration of medication if necessary.
Once the medication is injected, it works by blocking the nerves in the spinal cord, resulting in numbness and pain relief in the lower part of the body. This allows the patient to remain awake and alert while being free from discomfort.
Epidural anesthesia is known for its effectiveness in managing pain during labor and delivery, as well as providing relief for certain surgical procedures. It can be adjusted to provide different levels of pain relief, depending on the individual’s needs.
While epidural anesthesia is generally considered safe, there are potential complications that can arise. These may include a drop in blood pressure, headache, infection, or nerve damage. However, these complications are rare and can usually be managed by the healthcare team.
In summary, epidural anesthesia is a procedure that involves the administration of anesthesia into the epidural space to provide pain relief during childbirth or surgery. It is an effective method for managing pain and can be adjusted to meet individual needs. While there are potential complications, they are rare and can be managed by medical professionals.
What is Spinal Anesthesia?
Spinal anesthesia is a type of regional anesthesia that involves the injection of medication into the spinal canal. It is commonly used for surgeries and procedures below the waist, such as cesarean sections, hip replacements, and hernia repairs.
During a spinal anesthesia procedure, an anesthesiologist will administer the medication through a small needle inserted into the lower back. The medication numbs the nerves in the spinal cord, resulting in temporary loss of sensation and movement in the lower body.
Spinal anesthesia is different from epidural anesthesia, which involves the injection of medication into the epidural space surrounding the spinal cord. While both techniques provide pain relief, spinal anesthesia typically provides a more intense and rapid onset of numbness.
One of the benefits of spinal anesthesia is that it allows for a more complete block of sensation, making it an effective option for surgeries that require a high level of anesthesia. Additionally, spinal anesthesia is associated with fewer complications compared to general anesthesia.
However, like any medical procedure, spinal anesthesia does carry some risks and potential complications. These can include headache, infection, nerve damage, and allergic reactions to the medication. It is important to discuss these risks with your anesthesiologist before undergoing the procedure.
In conclusion, spinal anesthesia is a type of regional anesthesia that involves the injection of medication into the spinal canal. It provides effective pain relief and is commonly used for surgeries and procedures below the waist. While it has benefits and risks, it is a valuable tool in the field of anesthesia.
Differences between Epidural and Spinal Anesthesia

Spinal anesthesia and epidural anesthesia are both methods used to provide pain relief during medical procedures. While they are similar in some ways, there are key differences between the two.
Spinal anesthesia involves the injection of a local anesthetic into the cerebrospinal fluid in the spinal canal. This numbs the nerves in the lower half of the body, resulting in pain relief. The injection is typically done in the lower back, and the effects are felt quickly.
Epidural anesthesia also involves the injection of a local anesthetic, but it is administered into the epidural space, which is outside the spinal canal. This numbs the nerves in a larger area, providing pain relief for a longer duration. The injection is usually done in the lower back, and it may take a bit longer for the effects to be felt.
One of the main differences between the two methods is the extent of numbness they provide. Spinal anesthesia typically results in a more complete numbness, as it directly affects the nerves in the spinal canal. Epidural anesthesia, on the other hand, may not provide as complete of a numbness, as it affects a larger area and may not reach all the nerves.
Another difference is the potential for complications. Spinal anesthesia carries a slightly higher risk of complications, such as headaches or nerve damage. Epidural anesthesia, while generally considered safer, can still have complications, such as infection or bleeding.
The procedure for administering spinal anesthesia involves a single injection into the spinal canal. The effects are usually felt quickly, and the numbness can last for a few hours. Epidural anesthesia, on the other hand, involves the placement of a catheter into the epidural space, allowing for continuous administration of the anesthetic. This can provide pain relief for a longer period of time.
In summary, spinal anesthesia and epidural anesthesia are both effective methods of pain relief during medical procedures. Spinal anesthesia provides more complete numbness but carries a slightly higher risk of complications. Epidural anesthesia provides pain relief over a longer duration but may not provide as complete of a numbness. The choice between the two methods depends on the specific procedure and the preferences of the patient and healthcare provider.
Administration
The administration of an epidural or spinal involves a similar procedure. Both are typically performed by an anesthesiologist, a specialized doctor who is trained in administering anesthesia.
During an epidural, the anesthesiologist will insert a thin catheter into the epidural space in the lower back. This space is located just outside the spinal cord and contains nerves that transmit pain signals. The catheter is then used to deliver medication, usually a combination of a local anesthetic and a pain-relieving opioid, through an injection. This medication helps to numb the nerves and block pain signals, providing pain relief in the lower body.
On the other hand, a spinal involves a single injection of medication directly into the cerebrospinal fluid in the spinal canal. This medication also includes a local anesthetic and a pain-relieving opioid. The injection is usually made in the lower back, below the level of the spinal cord. The medication then spreads throughout the cerebrospinal fluid, numbing the nerves and providing pain relief.
Both procedures are generally safe, but there can be complications. With an epidural, there is a small risk of complications such as infection, bleeding, or nerve damage. The catheter can also become dislodged, requiring repositioning. With a spinal, there is a risk of headache, infection, or nerve damage. However, these complications are rare and can usually be managed by the anesthesiologist.
In summary, the administration of an epidural or spinal involves the insertion of a catheter or a single injection of medication by an anesthesiologist. Both procedures aim to provide pain relief by numbing the nerves. While there can be complications, they are generally rare and can be managed by the medical professional.
FAQ about topic Epidural vs Spinal: Understanding the Differences and Benefits
What is the difference between an epidural and a spinal?
An epidural and a spinal are both types of regional anesthesia used during childbirth or surgery, but they differ in the way they are administered. An epidural involves inserting a catheter into the epidural space in the lower back, while a spinal involves injecting medication directly into the cerebrospinal fluid in the spinal canal.
Which type of anesthesia is more effective for pain relief during childbirth?
Both epidurals and spinals are effective for pain relief during childbirth, but epidurals are typically preferred because they provide continuous pain relief throughout labor. Spinals are often used for cesarean sections or when a shorter duration of pain relief is needed.
Are there any risks or side effects associated with epidurals and spinals?
While epidurals and spinals are generally safe, there are some risks and side effects to consider. These can include a drop in blood pressure, headache, infection, nerve damage, and difficulty urinating. It’s important to discuss these risks with your healthcare provider before choosing anesthesia.
Can I choose between an epidural and a spinal for my childbirth?
In most cases, the choice between an epidural and a spinal is made by the healthcare provider based on the specific circumstances of the childbirth. However, if there are no medical contraindications, you can discuss your preferences with your healthcare provider and they will take them into consideration.
How long does the pain relief last with an epidural compared to a spinal?
The duration of pain relief with an epidural can vary, but it typically lasts throughout labor and delivery. On the other hand, the pain relief from a spinal usually lasts for a shorter duration, typically a few hours. The healthcare provider will determine the best option based on the expected duration of pain relief needed.
What is the difference between an epidural and a spinal block?
An epidural block involves the injection of medication into the epidural space, which is the space surrounding the spinal cord. A spinal block, on the other hand, involves the injection of medication directly into the cerebrospinal fluid in the spinal canal.
Are epidurals and spinal blocks used for the same purposes?
Both epidurals and spinal blocks are commonly used for pain relief during childbirth and certain surgical procedures. However, epidurals are also used for long-term pain management, while spinal blocks are typically used for shorter procedures.
What are the benefits of an epidural?
Epidurals provide effective pain relief during labor and delivery, allowing women to have a more comfortable birthing experience. They can also be used for postoperative pain management and chronic pain conditions. Additionally, epidurals can be adjusted to provide different levels of pain relief.
What are the potential risks and side effects of a spinal block?
Some potential risks and side effects of a spinal block include headache, infection, bleeding, nerve damage, and allergic reactions to the medication. However, these complications are rare and can be minimized with proper technique and monitoring.
Can anyone receive an epidural or spinal block?
Most people are eligible to receive an epidural or spinal block. However, there are certain medical conditions and medications that may increase the risks associated with these procedures. It is important to discuss your medical history and any concerns with your healthcare provider before receiving an epidural or spinal block.
I am Lena N. Blackwell, a passionate writer and the author behind the content you find on vpequipments.in.
My work covers a range of topics including babies, culture, food, garden, holidays, pregnancy, tips, and travel. I strive to provide valuable insights and information to help parents, families, and individuals navigate through various aspects of life. My goal is to create content that is not only informative but also engaging and relatable, making your journey a little bit easier and more enjoyable.